Luxury Facilities at the Canadian Centre for Addiction
If you’re going through a tough time with drug addiction, you don’t have to face it alone. Our Luxury Rehab Centres in Port Hope and Cobourg, Ontario, are quiet, comfortable places where you can take a real break and start fresh. Both locations support people seeking opioid rehab, with discreet intake, medical oversight, and a plan tailored to your goals.
In Port Hope, our private rehab centre feels more like a peaceful retreat. Every room has calming lake views, a fireplace, and multiple decks to relax on. It’s a space to breathe, slow down, and focus on getting better. Alongside fresh, 5-star meals prepared by our chef, you’ll have access to on-site clinicians who understand opioid withdrawal – fatigue, low mood, sleep disruption – and how to manage it safely.
Over in Cobourg, the vibe is just as warm and welcoming. It’s a place where you’ll be supported by people who truly care. We’re here to listen, guide you, and help you feel more like yourself again. Your care may include cognitive behavioural therapy, motivational interviewing, and contingency management – approaches shown to help with opioid abuse.
Each rehab treatment program includes one-to-one therapy, small group work, family support when helpful, and a relapse-prevention plan you can actually use at home. We also coordinate gradual return-to-work strategies for people with heroin or fentanyl addiction, boundary setting, and healthy routines, so you leave with tools that last. And when you’re ready to step down, we help you transition to aftercare and community supports, ensuring the next part of your recovery is steady, informed, and supported.
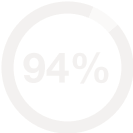 Success Rate:
Read Now
Success Rate:
Read Now











